Saliva is nature’s most effective protective strategy for your mouth. Resting saliva has a pH of about 6.75 and stimulated saliva has a pH of 8.0. When we begin to look at things that threaten this protection there are several that come to mind.
1. Medication Induced Xerostomia
70% of Americans take at least one medication daily, across all age demographics. Unfortunately I can’t take my patients off of their medications. So my job is to help them understand how it relates to their caries risk. I also let them know how much more susceptible they are when eating and drinking. I encourage them to keep their mouth moist and stay hydrated.
Abstract
OBJECTIVE:
Adolescents with psychiatric conditions may be at risk for xerostomia. In this preliminary study, we estimated xerostomia prevalence in adolescents ages 9 to 17 years from an inpatient psychiatric clinic (N = 25) and examined whether: (1) gender and age were associated with xerostomia and (2) xerostomia was associated with self-reported cavities.
METHODS:
We used a modified 11-item Xerostomia Index to identify xerostomia (no/yes) and asked if adolescents ever had or currently have cavities (no/yes).
RESULTS:
The mean age was 14 years (SD = 2.3) and 72% were male. Sixty percent reported xerostomia (SD = 50). There were no significant associations between xerostomia and gender (p = 0.99) or age (p = 0.66), or between xerostomia and past (p = 0.26) or current cavities (p = 0.11). Larger proportions of adolescents with xerostomia reported previous and current cavities.
CONCLUSIONS:
“Sixty percent of adolescents from an inpatient psychiatric clinic reported having xerostomia, which may lead to increased caries risk over time. Additional research should examine the prevalence and consequences of xerostomia in high-risk adolescents.”(Kaur M, Himadi E, Chi DL. Prevalence of xerostomia in an adolescent inpatient psychiatric clinic: A preliminary study. Spec Care Dentist. 2015 Dec 21. doi: 10.1111/scd.12154. [Epub ahead of print])
2. Sjogren’s Syndrome
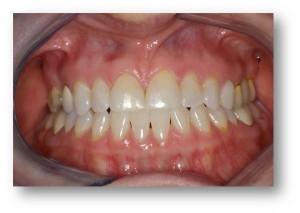
The photo is of a patient who was averaging 2 new caries a year, yet had impeccable home care. Her issue was she had virtually no saliva.
Abstract
BACKGROUND:
As North Americans live longer, have more chronic conditions and take more medications, adverse oral events are likely to increase and aggravate the symptoms of Sjögren syndrome (SS).
METHODS:
A total of 151 adults who self-reported having SS and who had a mean (standard deviation [SD]) age of 65.8 (11.5) years completed a survey that included questions about basic demographic information, current medical conditions, medications used (prescription and over the counter [OTC]) and the use of oral products to manage SS symptoms. Owing to the self-reporting process in our survey, the term “SS” in our study population represented a mixture of people with SS and people with dry mouth symptoms.
RESULTS:
The mean (SD) number of daily medications recorded as prescription, OTC and oral care products were 4.9 (3.5), 4.5 (2.8) and 4.6 (1.4), respectively. Participants with four or more comorbid medical conditions (n = 74; 49.0 percent) had significant differences (P < .05) in oral symptoms compared with those who had fewer than four (n = 75; 49.7 percent). Participants who were taking fewer than four prescription and OTC medications daily (n = 61; 40.4 percent) has significant differences (P < .05) in voice hoarseness compared with those taking four or more prescription and OTC medications daily (n = 54; 35.8 percent).
CONCLUSIONS:
The survey results indicated that medication use and comorbid medical conditions demonstrated significant differences and may have had a substantial impact on the oral symptoms in adults who self-reported having SS.
CLINICAL IMPLICATIONS:
Given the prevalence of SS, obtaining an accurate and complete medical and pharmacological history has implications for dental practitioners because medication use and comorbid medical conditions have a significant impact on oral symptoms in patients with SS.(Donaldson M, Epstein J, Villines D. Managing the care of patients with Sjögren syndrome and dry mouth: Comorbidities, medication use and dental care considerations. J Am Dent Assoc. 2014 Dec;145(12):1240-7. 151 Ad, >4 Rx)
3. Meth Mouth and Dental Caries
Abstract
BACKGROUND:
The authors used a large community sample of methamphetamine (MA) users to verify the patterns and severity of dental disease and establish a hierarchy of caries susceptibility by tooth type and tooth surface.
METHODS:
Using a stratified sampling approach, 571 MA users received comprehensive oral examinations and psychosocial assessments. Three calibrated dentists characterized dental and periodontal disease by using National Health and Nutrition Examination Survey protocols. The authors also collected data on substance use history and other attributes linked to dental disease.
RESULTS:
On all dental outcome measures, MA users evidenced high dental and periodontal disease, with older (≥ 30 years) and moderate or heavy MA users disproportionately affected. Women had higher rates of tooth loss and caries, as well as a greater prevalence of anterior caries. Current cigarette smokers were more likely to manifest 5 or more anterior surfaces with untreated caries and 3 or more teeth with root caries. Nearly 3% were edentulous, and a significant percentage (40%) indicated embarrassment with their dental appearance.
CONCLUSIONS:
MA users have high rates of dental and periodontal disease and manifest a dose-response relationship, with greater levels of MA use associated with higher rates of dental disease. Women and current cigarette smokers are affected disproportionately. The intraoral patterns and hierarchy of caries susceptibility in MA users are distinctive.
PRACTICAL IMPLICATIONS:
The prevalence and patterns of dental and periodontal disease could be used to alert dentists to possible covert MA use and to plan treatment. Concerns about dental appearance have potential as triggers for behavioral interventions. (Shetty V, Harrell L, Murphy DA, Vitero S, Gutierrez A, Belin TR, Dye BA, Spolsky VW. Dental disease patterns in methamphetamine users: Findings in a large urban sample.J Am Dent Assoc. 2015 Dec;146(12):875-85.)
4. Special Needs
Special needs individuals truly have special needs when it comes to dental caries. Under the direction of Drs. Steve Perlman and Allen Wong, CariFree has donated materials to begin studying these individuals and their caries needs at Special Olympics events. We are gaining the best ever data on this under served and often neglected and forgotten population.
“The subjects in this study had a high prevalence of dental caries and need for restorative care. They would benefit from parental education on diet modification, improvement of oral hygiene practices and regular dental visits.” (Oredugba FA, Akindayomi Y. Oral health status and treatment needs of children and young adults attending a day centre for individuals with special health care needs. BMC Oral Health October 2008. 22(8):30.)
